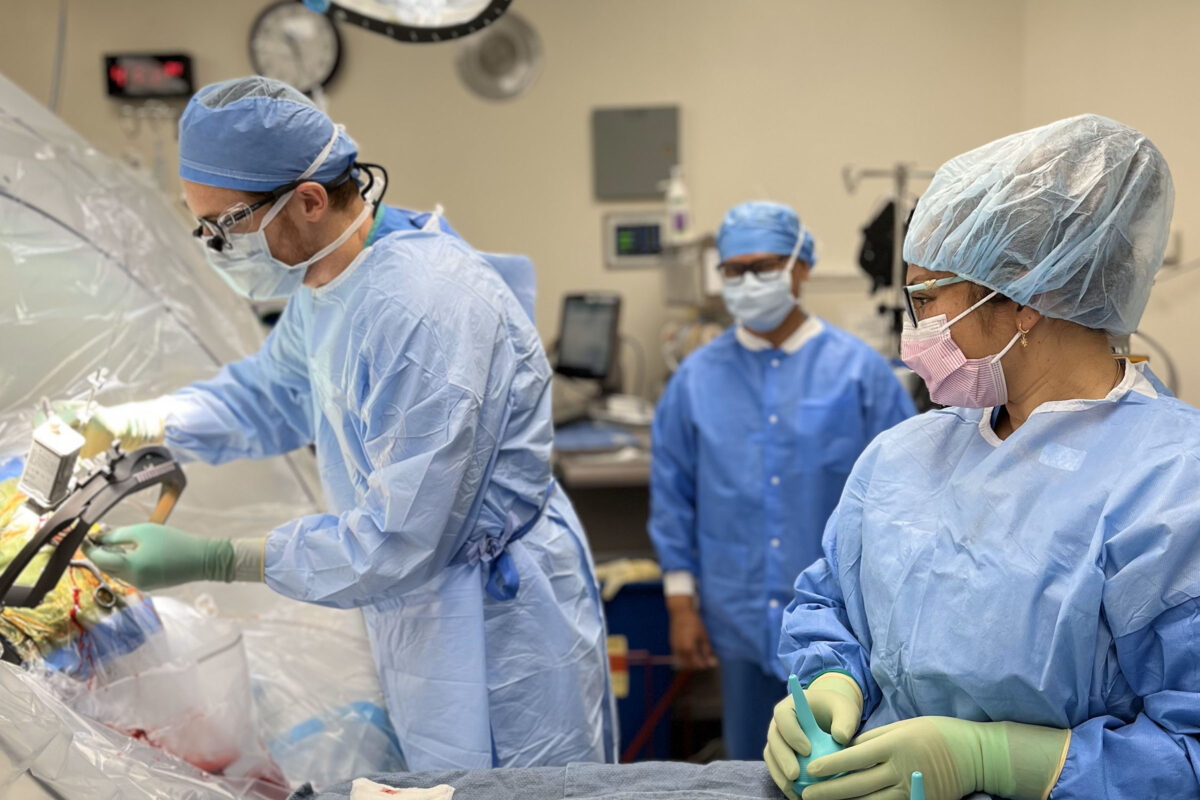
Deep Brain Stimulation (DBS), an advanced treatment for movement disorders like Parkinson’s disease, essential tremor, and dystonia, is now available at Kaiser Permanente in Sacramento. This procedure involves implanting electrodes in targeted brain regions to regulate abnormal activity through electrical impulses, offering patients improved quality of life and restored independence.
Implementing the DBS surgery program required strong interdisciplinary collaboration among physicians, nurses, surgical technicians, specialists, and department leaders. The outcome relies not only on surgical expertise but also on pre-and post-operative care, workflow optimization, and robust training.
Clinical nurses, nurse leaders, and Nursing Professional Development Specialists (NPDS) played a key role in implementing the DBS program. Amelia Dayucos, MSN, RN, CNOR, a Perioperative NPDS, led efforts to prepare staff for this new service. “When I first learned that this program was coming to Sacramento, I knew staff preparation would be critical. Our team worked on developing a comprehensive education program tailored to our staff’s learning needs,” she explained. She emphasized the importance of engaging clinical nurses in the process, noting, “Clinical nurses must be part of workflow design as experts in nursing care because they will use and execute the processes.”
Nurses, alongside their interdisciplinary partners, were instrumental in designing workflows, creating educational resources, and ensuring the best patient care. In the Operating Room, neurology nursing lead clinical nurses Earl Penalosa, BSN, RN, co-lead, Nancy Nguyen, BSN, RN, Surgical Tech Trevor Williams, OR Neuro Specialist Dustin Leyden, and Larry Bodden, MD, epilepsy neurosurgeon, conducted mock trial runs to optimize workflow, created detailed preference cards, visual board, and equipment use guides.
To guide post-operative care, Post Anesthesia Care Unit (PACU) clinical nurse Olga Bodnar, BSN, RN, and nursing team worked with Dr. Bodden, MD, to create pre- and post-operative workflows tailored to the procedure. The team also developed a checklist to guide the PACU nurses and streamline post-op care. In addition, the PACU education committee also led and implemented staff training sessions about DBS.
The interdisciplinary perioperative team’s work at Sacramento Medical Center has expanded Kaiser members’ access to DBS treatment. It also highlighted the critical role of nurses, from clinical to leadership, as leaders and change agents.